Getting Serious About Sepsis
By Trish Hughes Kreis for Assisted Living Directory
My introduction to Sepsis was during one of the first times my disabled brother was hospitalized with pneumonia. There was a flurry of activity in the Emergency Room, I heard the term “Sepsis” used with great concern and he was put in the ICU. Sepsis wasn’t explained very well to me but all the medical personnel stressed just how sick my brother was. Eventually Robert was moved into a regular hospital room where I asked one of the doctors about Sepsis. He dismissively told me it was common and many times followed pneumonia. He said it was nothing to be concerned about.
First, Trish talks about Sepsis: What is it, and how you can become the ‘expert’ about Sepsis in her video segment here:
In Robert’s case, which was it? Extremely concerning or nothing to worry about?
After doing my own research, I realized just how wrong the doctor was to be so dismissive about Sepsis. Sepsis is very serious and one of the leading causes of death in hospitals. I suspect the doctor was trying to ease my worries but not being forthcoming and blunt about the seriousness of Sepsis did me (and most likely his other patients as well) a huge disservice.
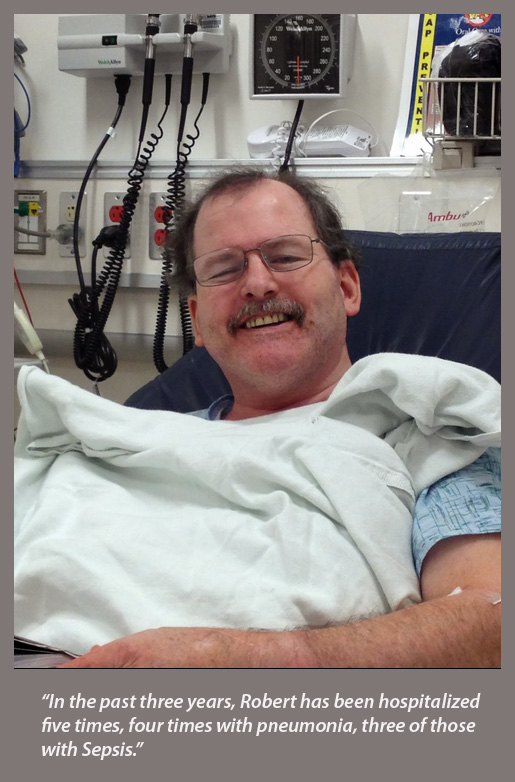
In the past three years, Robert has been hospitalized five times, four times with pneumonia, three of those with Sepsis. During one of the hospitalizations, Robert had gone into Septic Shock which is the most serious stage of Sepsis. It was a frightening experience (one in which the mortality rate is extremely high) and we were fortunate to see Robert pull through.
Many people are not aware of Sepsis until they or their loved one is in the hospital with a diagnosis of it. Knowing the symptoms and getting immediate treatment is essential to combatting this frightening condition. Unfortunately, there are still some doctors and hospitals who downplay the seriousness of Sepsis but armed with the following information, caregivers can advocate for their loved one to ensure swift and proper treatment.
These 11 tips will help take the fear out of the unknown.
- Symptoms. Chills that make a person literally shake and shiver, fever, extremely low blood pressure, extremely high pulse rate, altered mental state (which can include a decline in mobility/movement), extremely difficult to rouse, decreased urine output, shortness of breath and edema.
- Fever. It is important to know the baseline temperature of you or your loved one. For instance, a fever of 101° F is generally an indication of a severe infection. However, for those with a brain injury, the “normal” temperature is sometimes a full degree lower than what is considered normal. This means a high temperature is lower than what is typical.
- Risk Factors. The elderly or the very young, people with compromised immune symptoms, those with severe wounds, injuries or burns and those with catheters or breathing tubes are most at risk for developing infections that can lead to Sepsis.
- Precautions. Because Sepsis can come on quickly in some people (particularly the elderly or those with compromised immune systems), taking daily vitals will alert the caregiver to a change in baseline vitals.
- Be on Alert. Check vitals more frequently when your loved one is sick. Consult with a medical professional when there is a sign of a bad cold (which can turn into pneumonia), bladder or kidney infection or any other sort of infection. The key is to stop the underlying infection before Sepsis joins the party.
- Antibiotic Resistance. Many people have developed a resistance to some antibiotics (my brother is in this category). This increases the likelihood of developing bacterial infections that can trigger Sepsis. While there is not anything that can be done to reverse the resistance, knowing which antibiotics the patient is resistant to and sharing that information with medical personnel will give them valuable information in order to treat the underlying infection.
- Septic Shock. Septic Shock is the most severe form of Sepsis which can lead to organ failure and, possibly, death. As a caregiver, hearing the words “Septic Shock” can be very frightening but know this is not a death sentence. The mortality rate is high but swift treatment is essential and can be successful.
- Treatment. Sepsis will be treated with very strong antibiotics, usually in the ICU. The underlying cause of the infection will need to be detected (some examples are pneumonia, kidney infection, infected skin lesion). Fluids are also necessary in order to keep the organs working properly.
- Central Venous Catheter. When Robert was in Septic Shock, the ER personnel had to insert a “central line” in order to get his blood pressure up in as short of a time as possible. This is an IV line inserted into a large vein in the neck. I had never seen so many people work on him at once and it was extremely scary to watch. Just knowing this is a possibility might make the experience less scary.
- Information. The more information you have about Sepsis, the quicker you will be able to recognize it. The Sepsis Alliance Organization is a terrific resource for patients and their caregivers.
- Advocate. Are the medical personnel not recognizing signs of Sepsis? Advocate for yourself or your loved one. Medical personnel, particularly in the Emergency Room, are stretched thin and might need the caregiver asking questions and advocating and saying the word “Sepsis.” You know your loved one and their baseline health and behavior more than the ER doctors do. Do not be afraid to speak up.
Sepsis is something that is serious but that can be survived. Please share this information with other care providers, medical personnel in assisted living or skilled nursing facilities and anyone else who cares for others. It is essential to be well-prepared when faced with this serious condition.
Additional Advice: Families with seniors living in long-term care such as assisted living should ascertain whether the staff is knowledgeable, or trained in recognizing Sepsis, and how to handle it should it occur within the facility.